Doug Kerr
Well-known member
Part 1.
I have diabetes. An important aspect of managing my therapy is to be aware of my blood glucose concentration.
A common way to do that is with a "finger stick" glucometer. A lancing device pokes a small blade into the finger. The small drop of capillary blood that emerges is picked up by a disposable test strip inserted in the instrument. An ingenious electrochemical process allows the instyrument to measure the glucose concentration in this venous blood sample, which value tracks closely with the glucose concentration in arterial blood, the metric that is actually of interest.
But there are disadvantages. A small one is the nuisance of doing this perhaps before every meal and perhaps also at other times of the day. But the best understanding of the state of control of the patient's diabetes comes from knowing how the blood glucose concentration varies over the entire day. It is just not practical for the patient to, for example, measure his blood glucose concentration with a finger stick instrument every hour, certainly not overnight.
These limitations are overcome by continuous glucose monitor (CGM) systems. These typically have a small disposable sensor fasted by adhesive to the patient's skin. A small probe extends into the flesh, where it observes the interstitial fluid. Again an ingenious electrochemical system allows the sensor to determine the glucose concentration in the interstitial fluid, which value tracks closely with the glucose concentration in arterial blood, the metric that is actually of interest
The result is captured at short intervals, often by wireless transmission to a receiving device, which can even be a smartphone equipped with an appropriate app.
Such systems are made by several manufacturers.
For the past five years I have used a CGM system made by Abbott Laboratories, called the FreeStyle Libre 14 Day system. I have recently converted to a later generation product from the same company, the FreeStyle Libre 3+ system.
In the photos that follow, those that are my work carry the tag "dak" under them. The others are images found on the Internet, and are used here under the doctrine of fair use.
******
The sensor of the system is about the diameter of a nickel coin and only slightly thicker. We see it here with a nickel:

dak
We see the sensor as it would be seen in place on the patient. The recommended location is the back of the upper arm.
Here we see the opposite face of the sensor, the side that will be against the patient's skin, held by a disk of double sided adhesive tape with a very tenacious adhesive (not present here).
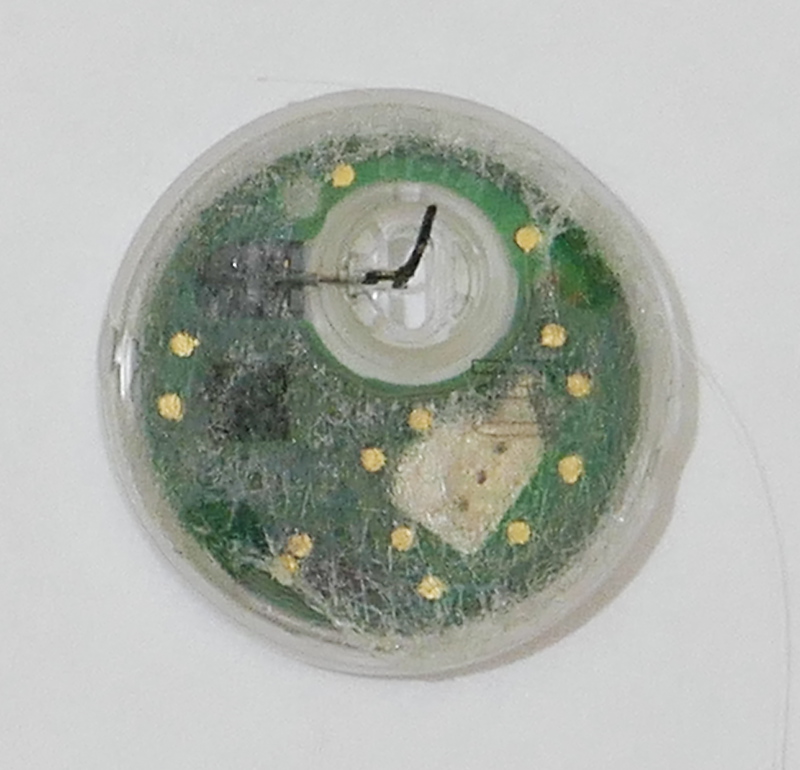
dak
We see projecting from the sensor the probe, which is highly flexible. When the sensor is applied, this probe is surrounded by an open sided steel "introduction needle" with a sharp tip. This will allow the probe to be pushed into the flesh, which we could not do with the bare probe (it being too "limp" for that). We see the introduction needle here:

dak
As soon as the sensor (and probe) is in place, that needle is extracted from around the probe and wholly out of the sensor.
[To be continued.]
I have diabetes. An important aspect of managing my therapy is to be aware of my blood glucose concentration.
A common way to do that is with a "finger stick" glucometer. A lancing device pokes a small blade into the finger. The small drop of capillary blood that emerges is picked up by a disposable test strip inserted in the instrument. An ingenious electrochemical process allows the instyrument to measure the glucose concentration in this venous blood sample, which value tracks closely with the glucose concentration in arterial blood, the metric that is actually of interest.
But there are disadvantages. A small one is the nuisance of doing this perhaps before every meal and perhaps also at other times of the day. But the best understanding of the state of control of the patient's diabetes comes from knowing how the blood glucose concentration varies over the entire day. It is just not practical for the patient to, for example, measure his blood glucose concentration with a finger stick instrument every hour, certainly not overnight.
These limitations are overcome by continuous glucose monitor (CGM) systems. These typically have a small disposable sensor fasted by adhesive to the patient's skin. A small probe extends into the flesh, where it observes the interstitial fluid. Again an ingenious electrochemical system allows the sensor to determine the glucose concentration in the interstitial fluid, which value tracks closely with the glucose concentration in arterial blood, the metric that is actually of interest
The result is captured at short intervals, often by wireless transmission to a receiving device, which can even be a smartphone equipped with an appropriate app.
Such systems are made by several manufacturers.
For the past five years I have used a CGM system made by Abbott Laboratories, called the FreeStyle Libre 14 Day system. I have recently converted to a later generation product from the same company, the FreeStyle Libre 3+ system.
In the photos that follow, those that are my work carry the tag "dak" under them. The others are images found on the Internet, and are used here under the doctrine of fair use.
******
The sensor of the system is about the diameter of a nickel coin and only slightly thicker. We see it here with a nickel:
dak
We see the sensor as it would be seen in place on the patient. The recommended location is the back of the upper arm.
Here we see the opposite face of the sensor, the side that will be against the patient's skin, held by a disk of double sided adhesive tape with a very tenacious adhesive (not present here).
dak
We see projecting from the sensor the probe, which is highly flexible. When the sensor is applied, this probe is surrounded by an open sided steel "introduction needle" with a sharp tip. This will allow the probe to be pushed into the flesh, which we could not do with the bare probe (it being too "limp" for that). We see the introduction needle here:
dak
As soon as the sensor (and probe) is in place, that needle is extracted from around the probe and wholly out of the sensor.
[To be continued.]
Last edited:
